When do I need a reverse shoulder replacement?
Arthritis:
The main indication for this surgery is shoulder arthritis in the presence of non-functional rotator cuff or when you develop a specific type of arthritis called cuff tear arthritis which is seen in long standing rotator cuff tears.
Large Irreparable Rotator cuff tears:
In some elderly patients with large cuff tears, this arthroplasty is done as it is associated with better outcomes than repair.
Fracture of Proximal humerus:
Some fracture patterns in elderly which cannot be fixed, will need reverse shoulder replacement.
What is reverse total shoulder replacement?
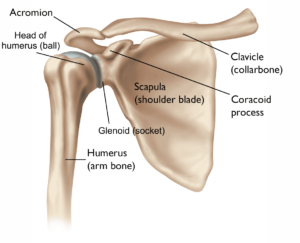
The shoulder joint is a ball and socket type of joint between the head of humerus (ball) and the glenoid (socket) and rotator cuff is a group of 4 tendons which helps in shoulder stability and movements. Reverse shoulder replacement is a specific type of shoulder replacement which is done for arthritis with a torn or non-functional rotator cuff.
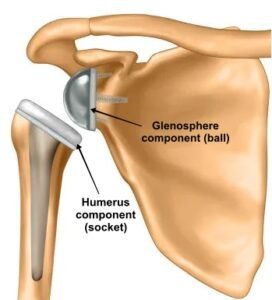
In this replacement the ball and socket components of the shoulder joint are reversed, meaning the artificial ball (Metal glenosphere) is attached to the shoulder blade (Glenoid) and the artificial socket is placed on the upper arm bone (humerus).
By reversing the ball and socket, the shoulder mechanics are altered, so that movements in the shoulder are possible even in the absence of rotator cuff.
Can you explain the procedure?
The surgery is done under anaesthesia (General or Regional block). The operation is done through a vertical incision over the front of the shoulder. The aim of the operation is to replace the diseased joint surfaces with artificial prostheses. The top of the humerus (the ball part of the joint) is replaced with a socket made from plastic and metal. The Glenoid (the socket part of the joint) is replaced with a metal half sphere.
What are the outcomes of the surgery?
Pain relief:
Most patients report substantial pain reduction, with studies indicating around 90-95% achieving excellent pain relief.
Functional improvement:
Patients generally see improvement in shoulder function, allowing them to perform daily activities with greater ease.
Range of motion:
While not always fully restored to normal, most patients experience improved range of motion, particularly in forward flexion, with the ability to reach overhead.
What are the common risks seen with this procedure?
- Infection
- Dislocation
- Fracture
- Stiffness
- Nerve injury
- Loosening – late complication.
What is the usual post-operative recovery timeline?
Length of hospital stay: Normally 2 to 3 days
Arm immobilisation: 4 weeks in sling or brace
Total recovery period: 3 – 6 months
Return to driving: 6 to 8 weeks
Return to work: Desk based job – 4 weeks, Manual job – 4 months
Key Points to Remember
- Consult a Specialist : A qualified orthopedic surgeon can accurately diagnose your condition and recommend the best treatment plan.
- Consider Non-Surgical Options : Physical therapy, medication, and lifestyle modifications may be sufficient for some conditions.
- Weigh the Risks and Benefits : Discuss the potential risks, benefits, and alternatives to surgery with your doctor.
- Ask Questions : Don't hesitate to ask your doctor any questions you may have about your condition and treatment options.
By working closely with your healthcare provider, you can make informed decisions about your knee health and choose the best course of action for your specific needs.
