What is osteoarthritis of knee?
Osteoarthritis is a degenerative joint condition where the cartilage covering the ends of bones in the knee joint gradually wears away, leading to pain, stiffness, and reduced movement in the knee. In a healthy knee joint, cartilage provides a smooth, cushion-like surface that lets the bones move against each other with minimal friction and absorbs shock during weight-bearing activities. With osteoarthritis, this cartilage becomes thinner and rougher, so the bones begin to rub more closely against each other resulting in pain, swelling and stiffness.
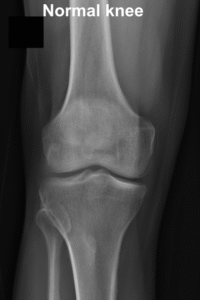
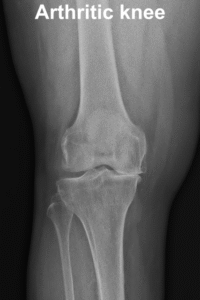
What are the risk factors?
Non-modifiable risk factors:
- Age: The risk increases as people get older.
- Gender: Females are more likely to develop knee osteoarthritis
- Genetics/family history: Having a family history of osteoarthritis increases individual risk.
- Bone deformities: Congenital joint or cartilage abnormalities also raise the risk.
Modifiable risk factors:
- Obesity: Excess body weight adds stress to knee joints, increasing risk.
- Knee injury: Prior trauma (such as sports injuries or accidents) increases the risk of developing knee OA.
- Occupation and repetitive stress: Jobs or activities that involve frequent kneeling, squatting, or repetitive stress on the knees heighten risk.
- Muscle weakness or imbalance: Weakness in muscles around the knee or poor joint support predispose to OA.
- Metabolic conditions: Diseases like metabolic syndrome are associated with higher OA risk.
What are the symptoms?
- Knee pain: Pain is often brought on or worsened by activity (walking, climbing stairs), but can also be present at rest or at night.
- Stiffness and Reduced range of motion
- Swelling and inflammation
- Grinding or crackling sounds (crepitus)
- Tenderness: Pain when pressing areas around the knee.
- Joint deformity or enlargement
- Difficulty performing daily activities
What are the causes of osteoarthritis of knee?
- Primary (Idiopathic) Knee Osteoarthritis:
Most commonly results from the gradual degeneration of joint cartilage due to aging and “wear and tear” over time.
- Secondary Knee Osteoarthritis:
Results from a known cause or contributing factor. Common examples include previous knee injuries, congenital or structural disorders of the joint and other diseases, such as rheumatoid arthritis, gout, hemochromatosis, metabolic disorders, or conditions causing abnormal cartilage or bone.
What are the steps to prevent getting osteoarthritis of knee?
To help prevent osteoarthritis of the knee, focus on controlling modifiable risk factors through weight management, exercise, injury prevention, and healthy lifestyle habits.
The following steps can substantially reduce risk:
- Maintain a healthy body weight: Even modest weight loss can significantly cut your risk.
- Exercise regularly: Safe, low-impact exercises (such as swimming, cycling, and walking) improve joint stability and decrease injury risk.
- Prevent joint injuries: Warm up properly before exercising, use protective gear or braces if needed. If an injury occurs, treat it promptly to prevent further damage.
- Protect your joints: Use good body mechanics, avoid repetitive heavy lifting, kneeling, or squatting, and practice good posture (stand straight, keep shoulders back, and avoid awkward joint positions).
- Eat a balanced diet: Diets rich in fruits, vegetables and low in processed foods and sugars can decrease inflammation and support joint health.
- Stay physically active: Physical activity helps keep joints lubricated, muscles strong, and body weight under control. Aim for about 30 minutes of moderate activity most days.
What are the non-operative methods available for the treatment of osteoarthritis?
- Physical Therapy and Exercise:
Strengthening muscles around the knee, especially the quadriceps, through low-impact exercises like walking, swimming, and cycling helps stabilize the joint, reduce pain, and improve mobility. Physical therapy can also include techniques like ice/heat application, electrical nerve stimulation, and balance training.
- Weight Management:
Losing excess body weight reduces stress on the knee joints and decreases inflammation, significantly lowering pain and functional impairment.
- Medications:
Nonsteroidal anti-inflammatory drugs (NSAIDs) can reduce pain and swelling. Some supplements like glucosamine sulfate and hyaluronic acid are also used.
- Intra-articular Injections:
These include corticosteroid injections or hyaluronic acid (lubricant) or platelet-rich plasma (PRP) injections to decrease inflammation and pain, to lubricate the joint and enhance mobility.
- Assistive Devices and Bracing:
Knee braces, shoe inserts, or walking aids can offload stress on affected parts of the knee, improve alignment, and enhance stability.
- Electrotherapy and Other Modalities:
Transcutaneous electrical nerve stimulation (TENS), diathermy, and other physical modalities may provide symptom relief.
What are the surgeries done for the treatment of osteoarthritis?
The main surgeries done for knee osteoarthritis can be broadly classified into knee-preserving and knee replacement surgeries.
Knee-Preserving surgeries:
These are mainly indicated in milder early osteoarthritis and also to correct the risk factors of OA. They have no role in advanced or severe osteoarthritis.
- Arthroscopic knee debridement: This minimally invasive surgery involves cleaning out the joint by removing loose cartilage or bone fragments, smoothing rough cartilage, removing inflamed tissue, and flushing the joint.
- Cartilage repair surgery: Techniques aimed at repairing or regenerating damaged cartilage. This is useful in small areas of cartilage loss or damage. It is not useful in diffuse disease or advanced OA.
- Osteotomy: This surgery involves cutting and reshaping the bone near the knee (above or below the joint) to shift the weight away from the damaged part of the knee. It is usually recommended for younger, active patients with osteoarthritis limited to one side of the knee. Osteotomy can delay the need for knee replacement.
Knee-Replacement surgeries:
These are indicated in patients with moderate to severe osteoarthritis. It is one of the most common surgeries done in Orthopaedics.
- Unicompartmental (partial) knee replacement: Replacement of only the damaged compartment of the knee. Suitable for patients with OA affecting only one part of the knee.
- Total knee replacement (arthroplasty): Removal of the damaged knee joint surfaces and replacement with an artificial prosthesis. This is the most common surgical treatment for severe, advanced knee osteoarthritis, especially in older patients.
